Porous bones. That’s what the word osteoporosis means. We’ve come to associate it with the aged, especially women. Yet, osteoporosis affects men, women, even children, in all age groups. This decrease in bone density leads to bone fragility- they tend to break more easily!
Most people believe that bones are static. That, once you physically ‘grow up’, your bones grow and don’t change. Nothing could be further from the truth! Your bones are always changing.
There are three types of bone cells. The first are osteo blasts and they are the bone- forming cells. The second type, osteo cytes, maintain bones as a living tissue. They make up about 90% of the adult skeleton. The third kind, osteo clasts dissolve bone, breaking down calcium and phosphorous, and causing it to be reabsorbed. Lots of factors occur in this interplay of building and tearing down, especially hormones. So, your bones are dynamic, they grow and breakdown all the time.
Generally, up to about age 25, more bone mass build than broken down. At about age 30, the process begins to reverse and bone matter begins to disintegrate. The breakdown rate is about 0.3%-0.5% per year. However, women after menopause, can lose from 2%-3% per year! But, about half of bone mass disintegrate even before menopause!
Such a decrease leads to height loss, back and leg pain and more importantly, fractures! They can occur as the result of very minor trauma and are frequently in the vertebra. Known as compression fractures, they usually occur in the mid and lower back and can be due to just plain old gravity. There can also be numerous microfractures and about 35 percent of vertebral fractures are not painful.
However, they can accumulate and cause pain and disability. Also, once a vertebral fracture has occurred, the risk for further fractures becomes much higher.
Fractures can and do occur in other parts of the body, like the wrist. But the most common fracture associated with osteoporosis is the hip fracture, with often devastating consequences. In the first 12 months after a hip fracture, one person in five will die, one in two won’t be able to walk or perform the tasks of daily living without assistance and one in four will need extended aid in a long-term care facility like a nursing home.
Overcome Osteoporosis
The key to overcoming the dire consequences of osteoporosis is prevention, and that well before the time of menopause. And the single most important factor in prevention is exercise, particularly weight training. Putting a stress on the bones, like with weights, causes the body to respond by increasing bone density (or, at the minimum, reducing the rate of its dissolution).
It also stimulates the release of hormones that have positive influences on bone growth. While nobody is suggesting you take up bodybuilding, a well-rounded exercise program that includes weight training is an essential component in deterring osteoporosis. Sedentary lifestyles, coupled with poor nutrition, are the absolute worst things for your bones, not to mention your other body systems! Other lifestyle changes that will also help include quitting smoking and reducing your caffeine and alcohol intake.
Preventing It
Moreover, nutrition is really the other part of the equation. A healthy diet of green leafy vegetables (like kale and dandelion leaves), seaweeds (like nori), milk, cheese (particularly goat’s cheese), yogurt and kefir, tahini, fish (especially sardines and salmon) and grains, like oatmeal, all with as little added chemicals and preservatives as possible, constitutes the absolute barest minimum standard. Yogurt and kefir are especially utilizable by the body.
Some greens however, are harmful. They are mostly those high in oxalic acid and include swisschard, beet greens, spinach and rhubarb. Phosphorus-rich foods, including carbonated drinks, processed white flour products as well as many other processed foods, inhibit calcium uptake and utilization, and should be avoided. Those who down lots of soft drinks are four times more likely to break a bone!
Healthy bones need minerals, including calcium, phosphorus, potassium, manganese, magnesium, silica, iron, zinc, selenium, boron, sulphur, chromium, and a couple of dozen others. In order to adequately assimilate these minerals, we also need proteins, high-quality fats like fish oil and vitamins!
Calcium, however, is by far the most important of the minerals. Most adult women should be getting 1,000 mg a day or more before menopause and more afterwards. While milk has been promoted as the best source of calcium, it’s really not the case. An 8 oz. glass of milk does contain about 300 mg of calcium. But it’s not only how much you get but how much is used and the calcium in milk isn’t well absorbed. It’s the same problem with a lot of calcium supplements.
Important Supplements
Unfortunately, with today’s hectic schedules and over-filled lives, relying solely on diet is unrealistic and supplementation becomes necessary.
There are many calcium supplements on the market today. Most commonly use calcium citrate, calcium carbonate and calcium from oyster shells in their formulations. But recent studies suggest that the best type of calcium supplement is a concentrate of microcrystalline hydroxiapatite (MCHC).
They have shown that the MCHC type can increase bone density by more than 6%, even where there is advanced bone loss. It also helps in healing fractures. In addition to the calcium, MCHC also contains protein and over 25 other required minerals.
Also high on the list of minerals is magnesium, necessary for the chemical reactions that form new bone, and manganese, needed to increase bone resistance to fractures.
Herbs & Vitamins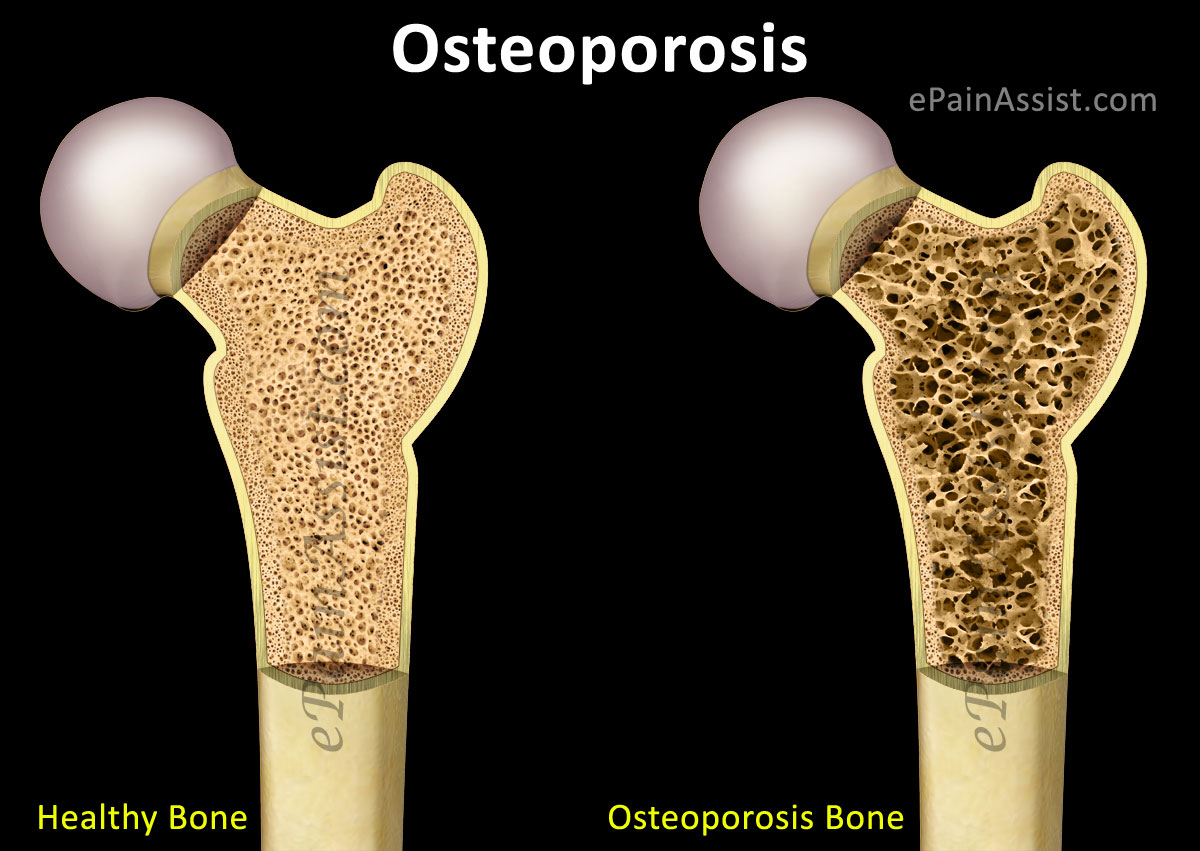
Vitamins are a crucial component of both bone growth and bone health. In particular, Vitamin D, which is so necessary for calcium absorption that it is added to milk, and Vitamin K, necessary to form osteocalcin , a protein found only in bone and required for bone formation.
Herbs can play a big role in bone health as well. Many herbs are rich in minerals, including calcium, and are extremely well absorbed.
They include stinging nettle (Urtica dioica), oatstraw (Avena sativa), red clover (Trifolium pretense), dandelion (Taraxacum officinale), Irish moss (Chondrus crispus) and especially horsetail (Equisetum arvense), which is high in silica and both strengthens bone and aids in healing fractures. However, if you have kidney problems, it is best to stay away from horsetail as it can be hard on the kidneys.
A Netherlands medical study determined that a minimum of 400 IU of Vitamin D and 80 micrograms of Vitamin K were necessary for optimum bone health in menopausal women.
The B vitamins are also very important for bones. Folic acid and Vitamin B6, for example, are necessary for the fibrous collagen framework onto which minerals deposit to make up the bone, while a vitamin B12 deficiency negatively impacts on proper osteoblast (the cells that form bone) functioning.
Allopathic Medications
On the allopathic side, the treatment of choice in menopausal women has been estrogen or hormonal replacement therapy. That’s because bone density decreases with the reduction of estrogen associated with menopause. But interestingly, a study done by St George’s Hospital Medical School at the University of London revealed that as the level of estrogen is reduced, the antioxidant level in the bone is also decreased.
When they introduced the antioxidants Vitamin C and N-acetyl cysteine, a form of the amino acid (the building blocks of proteins) cysteine, bone density began to increase! They had discovered the mechanism by which estrogen protects against osteoporosis and suggested an alternative to its controversial use.
Other medications commonly prescribed for osteoporosis include Fosamax (Alendronate) and Didronel (Etidronate) for both prevention and treatment. Also, Evista (Raloxifene), a relatively new drug that aids in preventing bone loss particularly in the spine, and Miacalcin (Calcitonin-salmon) which increases bone density up to 3% but appears to have little impact in reducing fractures.
The big problem with these drugs is the negative side-effects they can exhibit. Estrogen has been shown to increase the possibility of breast cancer by as much as 40%. Fosamex can cause esophogitis (inflammation of the esophagus) and even esophageal bleeding. Evista can have the relatively mild side effect of hot flashes but in some, the more serious complication of deep vein thrombosis (a blood clot in the deep veins).
Epidemic?
Osteoporosis is reaching epidemic proportions. In fact, the World Health Organization (WHO) has classified osteoporosis as the second leading health care problem after cardiovascular disease. Because of its usual long-term, asymptomatic onset, it is frequently referred to as the “silent epidemic”.
In the United States, some 6 million women over the age of 50 suffer from osteoporosis, while up to 17 million have low bone mass. Men do a little better with the statistics a little better than half that of women, probably because they have more bone mass to begin with.
Because it comes up on you slowly, take early heed. Put into action the suggestions outlined here and put yourself on the course to preventing what could otherwise be a debilitating life in the years that should indeed be golden!
This article is from Science’s archive and we’ve originally published it on an earlier date.
